|
Details of these papers are shown in table 4. No clinical trials were identified and all the papers available were case reports. AND Search outcomeĪltogether 51 papers were found of which six were deemed relevant. Medline 1966–02/03 using the OVID interface. You have heard of treatment with intravenous glucagon but wonder if it has been of any proved benefit. 
An ECG shows a sinus bradycardia of 50 bpm. She is bradycardic and hypotensive despite initial resuscitation with oxygen and intravenous fluids. No beta-blocker was mentioned in this case.A 25 year old patient presents to the emergency department two hours after taking a significant overdose of propanolol. 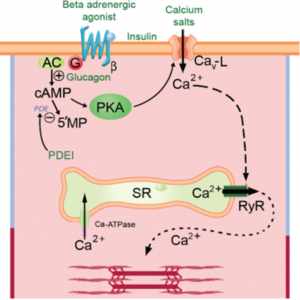 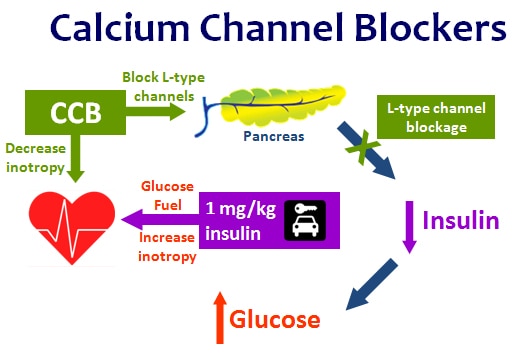
After epinephrine administration his blood pressure transiently rose to 280/110 mm Hg with subsequent anterolateral ST depressions. In a fourth case, a patient had anaphylaxis to radio-contrast media during elective coronary angiography.This suggests the need to use higher epi doses. Therapeutically, it acts as both an antagonist and antidote to benzodiazepines (particularly in cases of overdose), through competitive inhibition. A third case reported resistance to epinephrine in a patient on propranolol with anaphylaxis. Flumazenil (also known as flumazepil, code name Ro 15-1788) is a selective GABA A receptor antagonist administered via injection, otic insertion, or intranasally.She was administered epi and BP slowly normalized. In another case report, a patient on metoprolol (selective) developed anaphylaxis during elective laparoscopic cholecystectomy.There are also cases of vasospasm in patients not on beta blockers. Coronary vasospasm is a potential side effect when adding an agent with beta/alpha adrenergic properties (see cocaine literature), but it didn’t cause hypertensive crisis with reflex bradycardia. Afterward she had “normalization of BP” and then developed chest pain and a troponin leak. In one case report, the patient was on propranolol (non-selective) and had a blood pressure of 73/58 before epi.In fact, they point out that you may not see a response with epinephrine and suggest the possibility of needing a higher dose in patients on beta-blockers. The World Allergy Organization Guidelines on Anaphylaxis make no mention of adjusting epinephrine dose in various situations. So, what’s the answer? Is this really a concern? Should we be decreasing the epinephrine dose for anaphylactic patients on beta-blockers? Let’s take a closer look. 
This may be more pronounced in non-selective beta-blockers such as propranolol. The justification behind the ‘pearl’ is that giving epinephrine in the setting of beta-blockade may cause unopposed alpha-1 mediated vasoconstriction leading to hypertensive crisis and reflex bradycardia. Before I even started my search, I will admit my bias was to actually give more epinephrine to overcome the beta blockade. You might be asking why this ‘pearl’ has gained any ground considering it makes intuitive sense to actually need an INCREASED dose of epinephrine to overcome any preexisting beta-blockade. Patients on beta-blockers do have an increased risk for anaphylaxis, so there is a chance you’ll see a case just like this at some point. They asked a challenging question regarding a “pearl” they learned in which half-dose epinephrine should be administered in anaphylactic patients on beta-blockers. We therefore investigated hemodynamic effects and safety of highdose glucagon with and without concomitant betablockade. This paramedic was reviewing his anaphylaxis protocol with some new medics and providers. Intravenous highdose glucagon is a recommended antidote against betablocker poisonings, but clinical effects are unclear. Scott Weingart that someone had sent to him. Amal Mattu, Rob Orman, Mike Winters, and Haney Mallemat (just to name a few). I love when complex medication questions come across my desk from folks like Drs.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
